Artificial intelligence in healthcare is often talked about like a single destination: "AI + healthcare." But the healthcare system isn’t one customer, one workflow, or one dataset. It’s a network of players with different responsibilities, different incentives, and different kinds of data.
The first trap: treating healthcare like one user
If you’re building in this space, "healthcare" is not a persona.
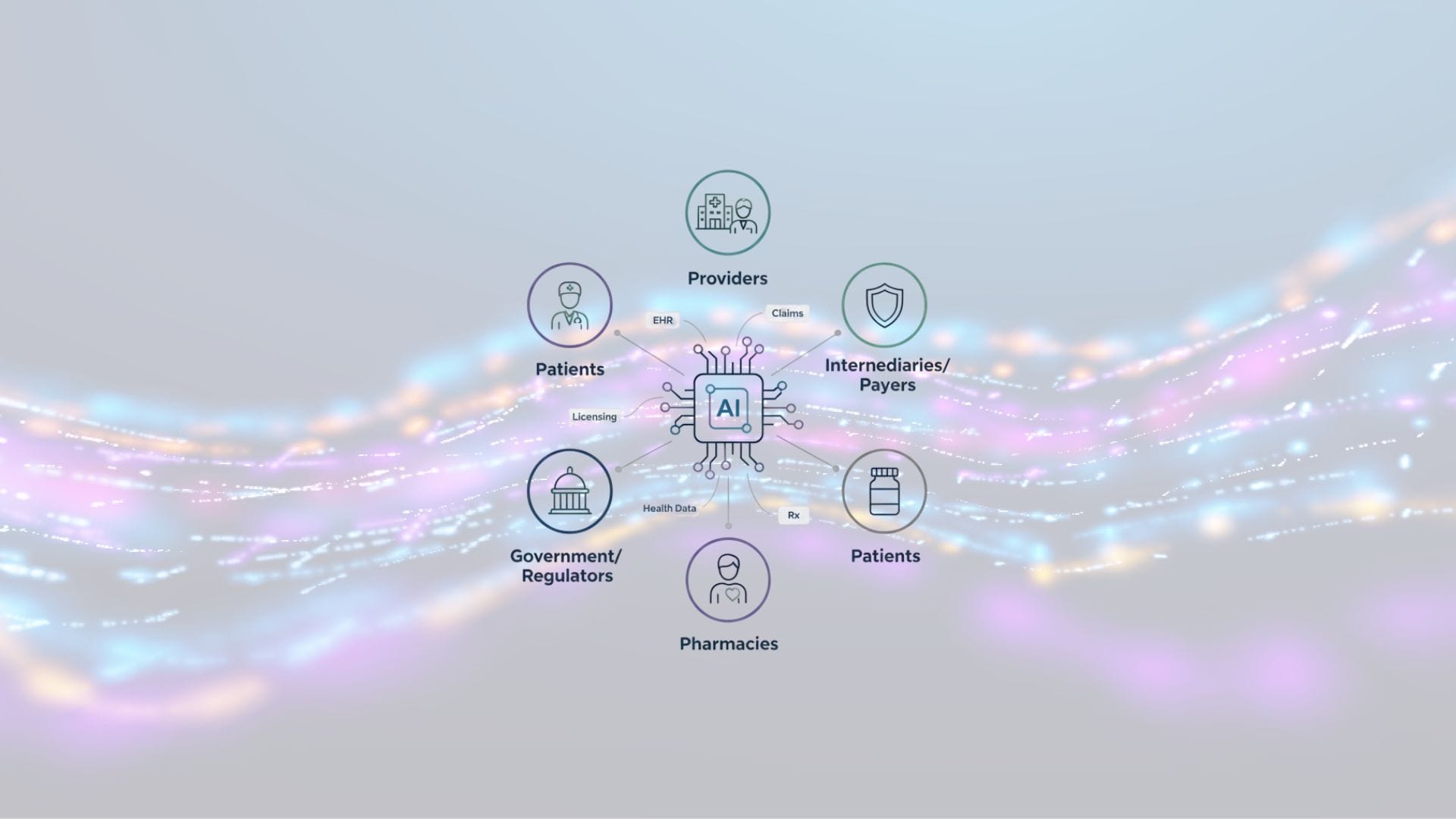
A health system has intermediaries, providers, patients, governments, pharmacies, and more each with their own goals. The right question is:
Who in the system will use the tool, and what do they get out of it?
If you can't answer that crisply, adoption becomes a guessing game.
1) Intermediaries (payers, plans, risk-bearing orgs)
Intermediaries typically have a defined population and a responsibility to manage risk and cost.
What they want from AI:
- Earlier signals that a health issue is emerging in their population
- Better outreach targeting (who needs help before a crisis)
- Risk management tools that help allocate resources to the right people at the right time
What motivates adoption:
- Reducing avoidable high-cost events
- Improving population outcomes
- Meeting performance/quality targets
2) Providers (clinics, hospitals, clinicians)
Providers are trying to deliver care while managing a constant firehose of information.
Where AI can help:
- Sorting and summarizing incoming patient information
- Supporting diagnosis and treatment planning
- Interpreting or triaging results (labs, imaging, consult notes)
- Identifying patients likely to need services soon, so care can be proactive
What motivates adoption:
- Better clinical throughput (without sacrificing quality)
- Reduced documentation burden
- Fewer missed signals
3) Patients (and patient-directed solutions)
Patients want to stay healthy, understand what’s happening, and decide when to seek care.
Where patient-facing AI fits:
- Symptom guidance and "do I need care?”"support
- Navigation: which service, where, when, and what to expect
- Coaching and adherence support (habits, meds, follow-ups)
What motivates adoption:
- Convenience
- Clarity
- Confidence in next steps
4) Governments and regulators
Governments regulate parts of the system and track what they regulate: facilities, licenses, compliance, reporting.
Potential AI uses:
- Monitoring safety/compliance signals
- Detecting patterns that require intervention
- Improving administrative workflows
5) Pharmacies and other operators
Pharmacies see medication dispensing data; other operators see other slices of reality.
AI value here:
- Safety signals (e.g., adherence gaps)
- Workflow optimization
- Patient support and navigation
The second trap: thinking "the data" is one thing
Once you pick a user, the next question is: what data do they actually have and why?
Different entities collect data for different reasons, and that shapes what the data looks like and what it’s good for.
Common healthcare data sources
Provider data: EHR (Electronic Health Records)
EHR data is built to help clinicians treat patients.
What it’s good at:
- Clinical detail: diagnoses, labs, vitals, notes, orders, imaging results (or references)
Common quirks:
- Lots of unstructured text (harder to normalize)
- Often incomplete for "business" questions like cost or payment
- Highly regulated because it's sensitive
Intermediary data: claims / payments / utilization
Intermediary data is built to pay for care and track services.
What it’s good at:
- A map of where patients received services
- Cost and utilization patterns across time and settings
Common quirks:
- Less clinical nuance than EHRs
- Collected for billing logic, not clinical reasoning
- Timing lags can be real (processing isn't instant)
Government data: licensing, facility registries, regulated services
What it’s good at:
- System-level oversight
- Compliance-related visibility
Common quirks:
- Often structured, but not designed for clinical prediction
- May be fragmented across agencies and jurisdictions
Pharmacy data: dispensed medications
What it’s good at:
- Medication fill patterns
- Refill timing and adherence proxies
Common quirks:
- Doesn’t guarantee ingestion (filled ≠ taken)
- Limited view outside medication activity



Comments